The Effects of Incomplete Surface Wetting
By Martin Conway
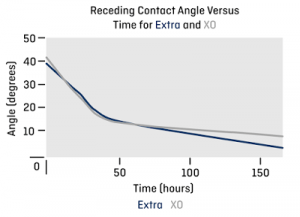
A modern GP material consists of a variety of monomers, some hydrophilic to enhance wettability and some silicone-based which boost oxygen flow, but they are inherently hydrophobic. The surface of a newly-lathed lens will consist of a random mixture of both hydrophobic and hydrophilic monomers. The wettability of the surface will not be at its best at this time because of the presence of the hydrophobic monomer at the surface. When the lens is immersed in a wetting solution, the hydrophobic sections of the polymer turn away from the wet surface, whereas the hydrophilic ends of the polymer chain are attracted to the wetting agent and turn toward the surface. This process is shown in figure 1. Over time, the surface of the lens becomes increasingly wettable and the wetting angle of the surfaces continues to decrease over about a week. After this time, the surface of the lens has changed significantly. It now consists of mainly hydrophilic monomer and its wetting angle will have dropped from around 40 degrees to 3 degrees in the case of Optimum Extra.
This change in the surface characteristics of the lens will have a significant impact upon not only the wearing comfort of the lens but on the propensity of the surface to collect lipid deposits. If the surface is wet then lipids, which are hydrophobic, will not adhere to the wet surface.
This is why labs are instructed to deliver GP lenses in a wetting solution. In the 48 hours that it takes the lenses to arrive at the practitioner’s office approximately half of the change in surface wettability will have taken place, and the lenses will be far more comfortable than if they had arrived dry. Even so, some patients will still notice the difference in comfort between an existing lens and the new replacement lens. They should be warned that the lens will continue to be conditioned over the next week and that comfort will improve. During this time, it is important that the patient is advised to use a surfactant cleaner on the lens after every wear.
If the patient fails to clean the lens properly and lipid is allowed to remain in contact with the lens overnight, the reverse of the process described above can take place. The lipid, which is hydrophobic, attracts the hydrophobic blocks of the polymer chain back to the surface and repels the hydrophilic blocks. The surface in contact with the lipid can become hydrophobic in a very short time.
In order to demonstrate the effect that lipid contamination can have on an otherwise hydrophilic surface, we devised an experiment to simulate what happens when lipid is left on the lens for a few hours without removal.

A fully wetted scleral lens was removed from a fitting set and blob of grease place on the surface.

The lens was then soaked in a storage solution for just 6 hours – less than would be the case during normal overnight storage.
The lens was then removed from the storage solution, cleaned with a surfactant cleaner to remove any visible trace of the grease and then worn.
Despite the lens looking clean through the slit lamp, the area under the grease is clearly not wetting. This area is repelling the tear film, but during the day’s wear would allow the lipids in the tear layer to adhere and build up again.
It is important that both labs and practitioners are aware of the fact that the surface of a modern GP material can be changed by its immediate environment. It is probably even more important to realise that this process is reversible.
We cannot rely upon patients to be compliant, particularly existing wearers who have perhaps worn lenses for years. By being aware of the factors controlling the performance of modern lenses, perhaps we can manage our patients a little better, to prevent unnecessary return and remakes of perfectly good lenses.

Martin Conway has over 40 years’ experience in the contact lens field as a qualified Contact Lens Optician. He is registered with the UK General Optical Council on the Speciality Contact Lens Register. Martin is a fellow of the British Contact Lens Association (FBCLA), and The International Association of Contact Lens Educators (FIACLE). He has served in the Professional Services role as an educator and clinical adviser on behalf of both Sauflon and CIBA, and now acts as Professional Services Consultant for Contamac. Martin has lectured extensively in Europe, Asia, Russia, North and South America and the Middle East.
