Support Healthy Lens Wear
by Dr Mile Brujic, OD, FAAO
It is incumbent upon the clinician fitting specialty lenses to be remarkably cognizant of the nuances that exist in promoting a healthy ocular surface. A healthy ocular surface provides the patient with the best chance to wear contact lenses comfortably and successfully. Optimized comfort in lens wear is a combination of optimizing the contact lens properties to promote comfort in addition to optimizing the ocular surface health to promote the best lens wearing experience possible.
The ocular surface isn’t just simply the conjunctiva and the cornea. The ocular surface includes the tear film that nourishes the conjunctiva and cornea. Increasing evidence is demonstrating that individuals who are having difficulties with contact lens wear may also have an underlying ocular surface disease that may be compromising comfortable contact lens wear.
In order to truly appreciate and respect the ocular surface’s influence on comfortable lens wear, it is incumbent upon the examiner to take special attention to many of the fine details of the ocular surface that are often revealing of abnormalities of normal health and physiology. Often we spend very little time examining these structures in our specialty lens wearers because of our increased attention to the characteristics of the lens fitting relationship.
The lid margin is critical as they not only block foreign substances from entering the eyes through the physical barrier of the eyelashes but they also maintain a healthy biofilm on the lid margin that allows the appropriate secretion of meibum from the meibomian glands. In a normal individual, low levels of bacteria are present at the lid margin and act in a symbiotic manner with the patient. These populations are normally kept in check and do not overpopulate the lid margin.
When the balance that exists at the lid margin with the bacteria is disrupted and bacteria overpopulate the lid margin, we can see the early signs of this as edema at the base of the lashes known as a volcano sign. Where we typically expect to see the skin either level or involuting at the base of the lash we actually see the skin tenting up at the base of the lashes. This is the first indication that bacteria are overpopulating the lash follicles causing localized inflammation within the follicles.
As these bacterial populations continue to overpopulate the lid margin, we begin to see the clinical manifestations much more readily apparent at the slit lamp as deposits and debris at the base of the lashes. The deposits at the base of the lashes are a combination of bacterial secretions and byproducts of excessive bacterial waste. Eventually, this bacterial biofilm will continue to overpopulate the lid margin, ultimately migrating posteriorly towards the meibomian gland orifices. Over time, this can promote the obstruction of the meibomian glands, ultimately leading to obstructive meibomian gland dysfunction.
It is critical to identify early lid margin disease. In order to best identify individuals with lid margin disease that may affect comfortable contact lens wear, it’s important to very carefully assess both the upper and the lower lid margin for the presence of any signs of inflammation. I found that the best way to identify this in patients is to make sure that the examination of the lid margin is performed utilizing high magnification at the slit lamp. By doing so we will be certain not to miss any level of lid margin disease.
For new patients that are being fit with specialty lenses, it’s crucial to identify lid margin disease prior to the lens fit. If blepharitis isn’t treated proactively and appropriately, it may lead to contact lens discomfort and intolerance. In our quest to keep our specialty lens patients as comfortable as possible I feel it’s critical to identify lid margin disease as a risk factor for uncomfortable lens wear. We currently have phenomenal treatment options available for not only initially treating these individuals but also maintaining lid margin and ocular surface health.
Case In Point
A 44-year-old new female patient presented to our office wearing small diameter GP lenses to correct her keratoconus. Her chief complaint at the time of the visit was reduced comfort with her contact lenses throughout the day. Her best corrected visual acuity with the contact lenses was OD 20/25, OS 20/25. Anterior segment examination revealed moderate blepharitis with significant deposits at the base of the lashes OU (Figure 1). There was moderate stagnation of the meibomian glands upon attempted expression.
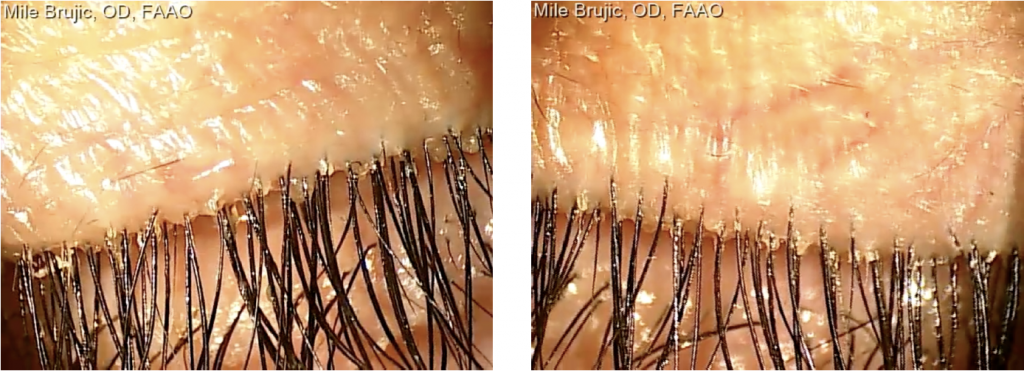
Figure 1. Moderate blepharitis with significant deposits at the base of the lashes OU.
We discussed the condition with the patient and also discussed options for vision correction. She preferred to proceed with a scleral lens fitting. We fit her successfully with scleral lenses utilizing a diagnostic fitting set and ordered the appropriate lenses from our specialty lens lab in the Optimum Extra material. Tangible Hydra-PEG™ was ordered for the lenses to optimize surface wettability. We also discussed blepharitis as a potential cause for the reduced comfort in the contact lenses. We photo documented the lid margin so that the patient could understand what was occurring and likely contributing to the reduced comfort in the contact lenses.
We put together a treatment plan which initially included a one-week course of a topical antibiotic-steroid combination drop that was to be used twice a day: once before the lenses were placed on the eyes in the morning and once after the lenses were taken out in the evening. The patient was instructed that after she put the drops in the eyes to close the eyes and then rub in any excess drops into the lid margin.
When the scleral lenses came in, the patient was scheduled for an appointment. At that visit, microblepharoexfoliation was first performed utilizing a Blephex. The lid margin was photo documented after the procedure to show the patient the improvement in the lid margin.
The new scleral lenses were placed on the eyes. Visual acuity through the lenses was OD 20/20 and OS 20/20. Optical coherence tomography images were taken of the corneal clearance and limbal clearance to assure an appropriate fitting relationship. The scleral landing zone was assessed at the slit lamp and found to be adequate. The patient was trained on appropriate insertion and removal of the lenses.
The patient was also given a bottle of HyClear to utilize twice a day. The patient was instructed to close the eyes before lens application in the morning, spray HyClear on the lid margin and rub it into the lash margin for approximately five to 10 seconds. She was instructed to do the exact same thing in the evening after lens removal.
HyClear is .01% hypochlorous acid and has strong levels of anti-microbial activity. It is an appropriate strategy for maintaining the health of the lid margins of these individuals for long periods of time. The importance of appropriate lid hygiene maintenance to prevent the return of excessive bacterial bioload at the lid margin was explained to the patient.
We saw the patient back for a one week follow up visit and the patient reported excellent visual acuity, and additionally, an extreme level of improved comfort with her contact lenses. She reported that she never remembered having this level of comfort with contact lenses before. We re-educated the patient on the importance of appropriate lid margin hygiene in order to promote healthy comfortable contact lens wear.
Six months after the initial visit we saw the patient back to follow up with the blepharitis and scleral lenses. The lid margin looked healthy OU and the patient reported good comfort and vision with the scleral lenses. (Figure 2) When questioned about the utilization of HyClear the patient reported good compliance with the treatment.
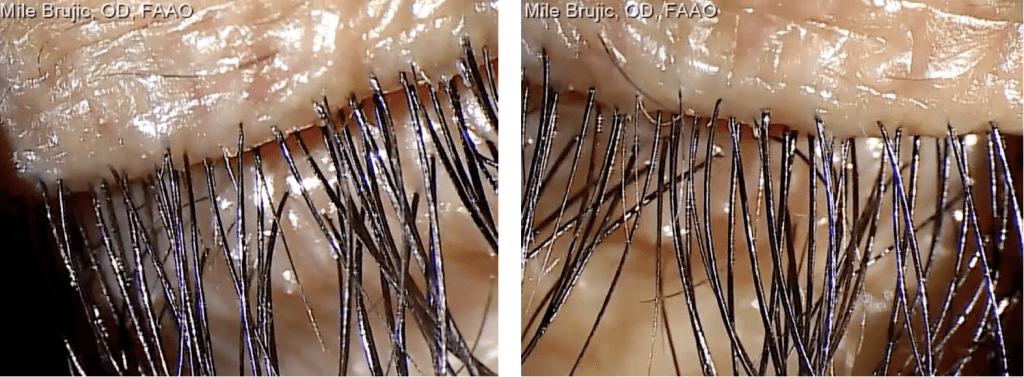
Figure 2. Six months follow up show healthy lid margin OU.
Appropriately identifying and treating lid margin disease is critical for our contact lens wearers. This is no more important for any other contact lens population than it is for our specialty lens wearing patients. These individuals are depending on us to make sure that we are creating the best wearing experience for them not only visually, but also in terms of the comfort that they experience while wearing their contact lenses. Through appropriate management of contemporary lens designs, in addition to managing the lid margin and ocular surface effectively, these patients are provided with the best opportunity for comfortable contact lens wear.
Thank you to Dr. Mile Brujic, O.D. for contributing to Global Insight.

Mile Brujic, OD, FAAO is a 2002 graduate of the New England College of Optometry. He is a partner of Premier Vision Group, a successful three location optometric practice in Northwest Ohio. He practices full scope optometry with an emphasis on ocular disease management of the anterior segment and specialty contact lenses. He has published over 250 articles and has given over 1400 lectures, both nationally and internationally on contemporary topics in eye care.
